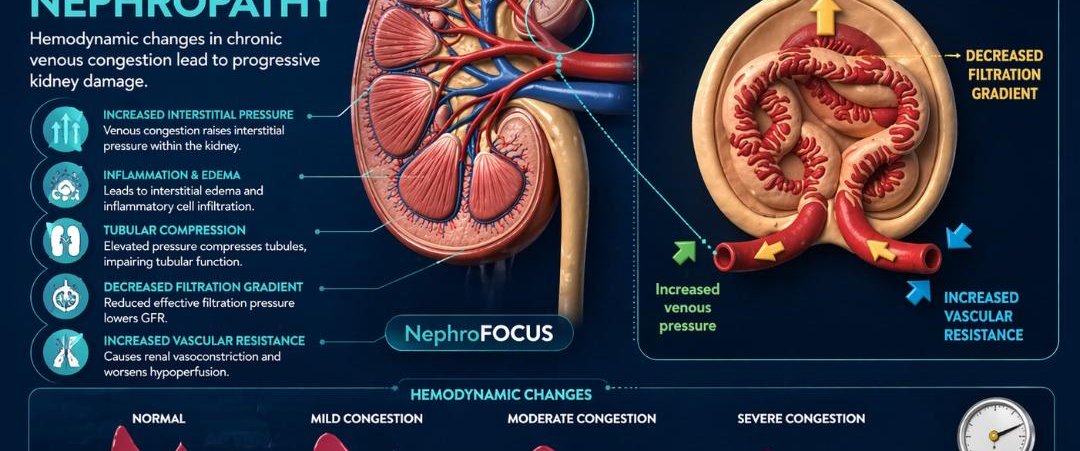
Hypertensive nephropathy is a major cause of chronic kidney disease (CKD) and contributes significantly to the burden of end-stage kidney disease (ESKD) worldwide.
Persistent elevation of systemic blood pressure causes progressive damage to the renal microvasculature, leading to nephron loss, declining glomerular filtration rate, and eventual renal failure if left untreated.
Early identification and evidence-based management are essential to slow progression.
Pathophysiology
Chronic hypertension leads to both structural and functional injury within the kidney.
Key mechanisms include:
- Hyaline arteriolosclerosis, causing narrowing of renal arterioles
- Reduced renal perfusion, leading to ischemic nephron injury
- Intraglomerular hypertension, causing glomerular hyperfiltration
- Progressive glomerulosclerosis and interstitial fibrosis
These changes result in irreversible nephron loss and gradual decline in renal function.
Risk Factors
Several factors increase susceptibility to hypertensive nephropathy:
- Long-standing uncontrolled hypertension
- Diabetes mellitus
- Advanced age
- Family history of kidney disease
- Smoking
- Dyslipidemia
- African ancestry
The coexistence of diabetes significantly accelerates renal decline.
Clinical Presentation
Hypertensive nephropathy often develops insidiously and may remain asymptomatic in early stages.
Common findings include:
- Gradual reduction in eGFR
- Mild to moderate albuminuria/proteinuria
- Persistent hypertension
- Evidence of hypertensive retinopathy
- Progressive CKD in advanced stages
Diagnostic Evaluation
1. Serum Creatinine and eGFR
Assessment of serum creatinine helps estimate the degree of renal impairment.
2. Urine Albumin-to-Creatinine Ratio (UACR)
Detection of albuminuria helps identify early renal damage.
3. Urinalysis
Proteinuria is usually present in non-nephrotic range.
4. Renal Ultrasound
In advanced disease, kidneys may appear small and shrunken due to chronic scarring.
Management Approach
5. Blood Pressure Control
Strict blood pressure control remains the cornerstone of management.
Target blood pressure is generally:
* <130/80 mmHg, particularly in patients with albuminuria
6. RAAS Inhibition
ACE inhibitors or ARBs are first-line therapies because they:
- Reduce intraglomerular pressure
- Decrease proteinuria
- Slow CKD progression
7. Lifestyle Modification
Non-pharmacological measures include:
- Sodium restriction
- Weight management
- Regular physical activity
- Smoking cessation
8. Glycemic Control in Diabetic Patients
Tight glucose control reduces progression risk.
In eligible patients with diabetic CKD, SGLT2 inhibitors provide additional renoprotective benefit.
9. Avoidance of Nephrotoxins
Avoid or limit exposure to:
- NSAIDs
- Contrast agents
- Other nephrotoxic medications
Monitoring
Ongoing follow-up should include:
- Serial eGFR
- UACR trends
- Blood pressure monitoring
- Electrolyte assessment
Without intervention, progression may lead to ESKD requiring dialysis or kidney transplantation.
Conclusion
Hypertensive nephropathy is a preventable but progressive cause of chronic kidney disease.
Early recognition of albuminuria, aggressive blood pressure control, RAAS blockade, and lifestyle modification remain essential in delaying renal decline and preventing progression to end-stage kidney disease.